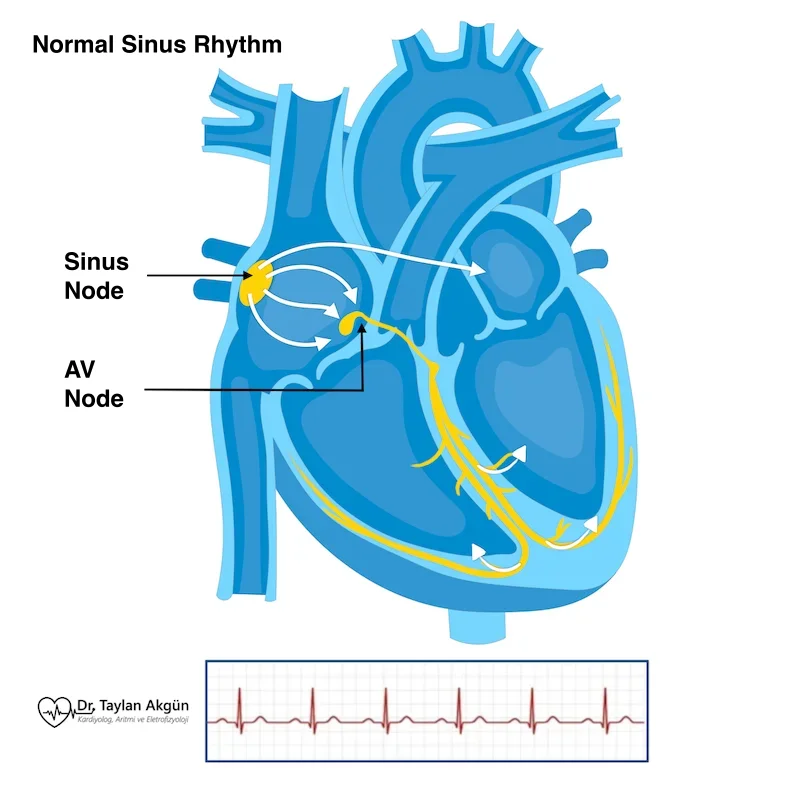
A heart attack and cardiac arrhythmias share a close, bidirectional relationship. A heart attack can trigger rhythm disturbances, and in some cases an arrhythmia may be the first sign — or the most dangerous consequence — of a heart attack. Understanding both conditions together is essential for comprehensive heart care.
Can a Heart Attack Cause Arrhythmias?
Yes. During a heart attack, part of the heart muscle is deprived of oxygen and sustains damage. This damage can affect the heart’s electrical system, disrupting its normal, coordinated rhythm.
During or immediately after a heart attack, palpitations, irregular heartbeat, extreme slowing, or dangerously fast rhythms may develop. Some arrhythmias are transient, while others are life-threatening and require urgent intervention. As a general rule, the greater the muscle damage, the higher the risk of rhythm disturbance.
Which Arrhythmias Occur After a Heart Attack?
Atrial fibrillation is among the most commonly seen arrhythmias following a heart attack. It causes irregular heartbeat and increases the risk of clot formation.
More dangerous are ventricular arrhythmias originating from the lower chambers of the heart. Ventricular tachycardia and ventricular fibrillation can suddenly impair the heart’s ability to pump blood and may lead to sudden cardiac arrest. These rhythms carry particular risk in the early phase of a heart attack.
Can an Arrhythmia Be a Sign of a Heart Attack?
Yes. In some patients, a heart attack does not present with classic chest pain but instead manifests as a sudden arrhythmia. Sudden palpitations, fainting, or abrupt loss of consciousness can be the first indication of an underlying heart attack.
This is especially relevant in older patients, those with diabetes, or individuals who have previously had a silent heart attack. For this reason, any new or suddenly developing serious arrhythmia should always be evaluated for a possible cardiac event.
Do Post-Heart Attack Arrhythmias Resolve?
This depends on the type of arrhythmia and the extent of myocardial damage. Some rhythm disturbances arise during the acute phase of a heart attack and resolve as the heart muscle heals.
However, if permanent damage has occurred, the arrhythmia may also become permanent. These patients may require long-term medication, rhythm-control procedures, or in some cases device-based therapies such as a pacemaker or implantable cardioverter-defibrillator (ICD).
Reducing the Risk of Arrhythmias After a Heart Attack
The most important strategy is protecting the heart muscle and reducing cardiac workload. Key measures include taking prescribed medications consistently, controlling blood pressure, cholesterol, and blood sugar, quitting smoking, and attending regular follow-up appointments.
In patients with significantly reduced heart muscle function, device therapy such as an ICD may be recommended as protection against life-threatening arrhythmias.