Tachycardia means a faster than normal heartbeat. In an adult at rest, the heart beats 60 to 100 times a minute. Any heart rate above 100 is called tachycardia. But this does not mean every fast heartbeat is a sign of illness. The heart is an organ that adjusts its speed to the body’s needs.
When you run, climb stairs, feel excited, run a fever, or drink coffee, your heart speeds up as expected. The body needs more blood at those moments, and the heart works faster to keep up. This is a natural response. The kind of tachycardia seen as a medical concern is when the heart beats fast at rest or for no clear reason.
What causes tachycardia?
The causes fall into two main groups. The first group covers fast heartbeats that come up as a response to something else going on in the body. Fever, anemia, an overactive thyroid, fluid loss, pain, stress, caffeine, and certain medications can all push the heart rate up. In these cases, the heart itself is not the problem. Once the underlying cause is treated, the heart rate settles on its own.
The second group comes from the heart’s own electrical system. The heart has a built-in electrical setup that controls each beat. When something goes wrong with this setup, the heart can start beating too fast for no good reason. This is an arrhythmia. Arrhythmia means a problem with the rhythm of the heart. Fast heartbeats from this group come from the heart itself and usually need their own treatment.
Types of tachycardia
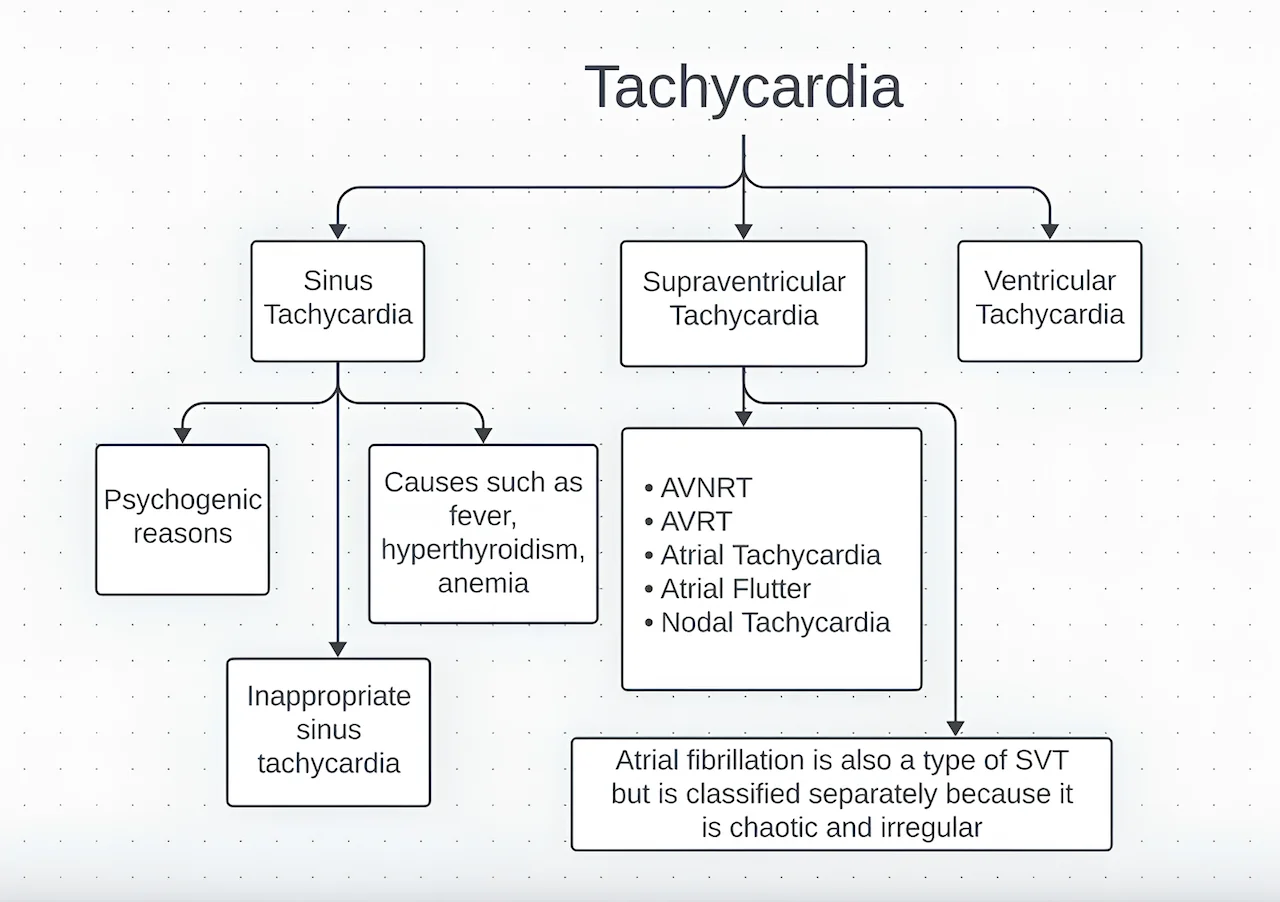
There is no single tachycardia. It is divided into types based on where in the heart the problem starts. This split shapes the treatment.
Sinus tachycardia is the most common type. It comes from the sinus node, the heart’s natural pacemaker. The sinus node is a small group of cells in the upper right chamber that starts each normal heartbeat. Sinus tachycardia is usually a response to something. It shows up with exercise, fever, excitement, or anemia. It is not dangerous and settles once the trigger is gone.
Supraventricular tachycardia is a sudden episode of fast heartbeats that starts in the upper chambers of the heart. Patients often describe it as “my heart sped up out of nowhere and then stopped just as suddenly.” An episode can last several minutes. It is rarely life-threatening but affects daily life and calls for treatment.
Ventricular tachycardia starts in the lower chambers of the heart. The ventricles are the large lower chambers that pump blood out to the body. This type is more serious. The heart beats fast and works less effectively at the same time. Symptoms tend to be heavier and the situation needs prompt attention.
Atrial fibrillation is also one of the most common reasons for a fast heartbeat. Here the upper chambers of the heart contract in a disorganized and uneven way. The rhythm is both fast and irregular. Atrial fibrillation has its own treatment approach.
What are the symptoms?
Some patients do not feel the fast heartbeat at all. It is found by chance during a blood pressure check or a routine exam. Those who do feel it often describe palpitations. They say things like “my heart is pounding,” “I can feel it in my chest,” or “my heart is fluttering.”
When the fast beat keeps going, the heart may not pump enough blood with each beat, and some parts of the body can get less blood. Lightheadedness, weakness, dimming of vision, shortness of breath, or a tight feeling in the chest can follow. In stronger episodes, fainting can occur.
How severe the symptoms feel depends on the type of tachycardia, how long it lasts, and whether the person already has a heart condition. A young, healthy person may handle a fast heart rate for a long time without much trouble, while someone with a known heart condition may struggle quickly.
Is it dangerous?
The answer depends on the type. Sinus tachycardia is almost never dangerous because it is just the body’s normal response. Supraventricular tachycardias are mostly not life-threatening either, but if left untreated, frequent episodes wear down quality of life.
Ventricular tachycardia is the type to watch closely. When it lasts long, it can seriously affect how well the heart pumps. So ventricular tachycardia with symptoms always needs medical review.
Atrial fibrillation is not always an immediate danger on its own. But in the long run, it can lead to clot formation and stroke, so its treatment is planned with care.
How is it diagnosed?
The first step is an ECG, also called an EKG. An ECG is a simple, painless test that turns the heart’s electrical activity into a recording. An ECG taken during the fast heartbeat usually shows the type of problem.
But episodes rarely happen during the office visit. By the time the patient arrives, things often look normal. In that case, a Holter monitor is used. A Holter is a small portable device that records every heartbeat for hours or even days while the patient goes about daily life. If an episode is caught, its type and details can be worked out.
For patients who need a closer look, an echocardiogram may be done. An echocardiogram is an imaging test that uses sound waves to show the structure of the heart. In some cases, an electrophysiology study is offered. This is a procedure in which thin wires are passed through a vein to study the heart’s electrical system in detail. Treatment can be done in the same session.
Treatment approach
Treatment is shaped fully by the cause. So talking about a single tachycardia treatment would be misleading.
When the fast heartbeat is a response to something else, the underlying cause is treated. Anemia is corrected, thyroid problems are managed, infections with fever are treated. Once the cause is gone, the heart rate returns to normal on its own.
When the source is the heart itself, things look different. If episodes are rare and mild, follow-up alone may be enough. For frequent episodes or those that disrupt daily life, two main options stand out. The first is rhythm-controlling medication. These reduce how often and how strongly the episodes happen. The second is catheter ablation. Ablation is a procedure that silences the small area causing the problem by delivering energy to it. A thin catheter is passed through a vein up to the heart, and the spot sending the wrong signal is taken out of action. Ablation offers a lasting fix in many types of tachycardia.
A few moves can help during an episode. Splashing the face with cold water, taking a deep breath and holding it, or bearing down can stop some supraventricular episodes. These are not right for every patient and should only be tried after a doctor has shown how.
When to call the doctor
A fast heartbeat that starts suddenly and keeps going, especially with dizziness, dimming of vision, chest pain, or fainting, calls for prompt review. For someone already known to have tachycardia, episodes that come more often, last longer, or feel stronger should also be looked at.
For people with a known heart condition, any new fast heartbeat needs to be checked. The course of the problem can be different in this group.
Frequently Asked Questions
My heart races when I get excited. Do I have tachycardia?
No. A faster heartbeat with excitement, fear, or exercise is normal. It is the bodys natural response. The kind seen as a medical concern is when the heart beats fast at rest, with no clear trigger.
My heart beats very fast during exercise. Is that a problem?
A higher heart rate during exercise is expected. It stays within a certain range based on age and fitness level. If even a short bit of exercise sends your heart racing, or if your heart rate stays high long after you stop, a check-up is a good idea.
Is tachycardia temporary or lasting?
That depends on the cause. Tachycardias linked to another condition in the body are temporary. Those coming from the hearts own electrical system tend to come back unless treated.
Can coffee or energy drinks cause tachycardia?
They can. Caffeine raises the heart rate in some people and can also set off existing rhythm problems. People who have episodes are advised to cut back on these drinks.
If I have tachycardia, will my blood pressure also rise?
Blood pressure can shift during an episode. In some people it rises, in others it drops. This depends on the type of episode and how long it lasts.
I am young. Can I have tachycardia?
Yes. Some types are seen mostly in young people and even in children. Age alone does not rule it out.
Will tachycardia be fully cured after ablation?
For many types, ablation gives a lasting solution. The success rate varies by type. Your doctor will share what to expect for the specific kind of tachycardia you have.